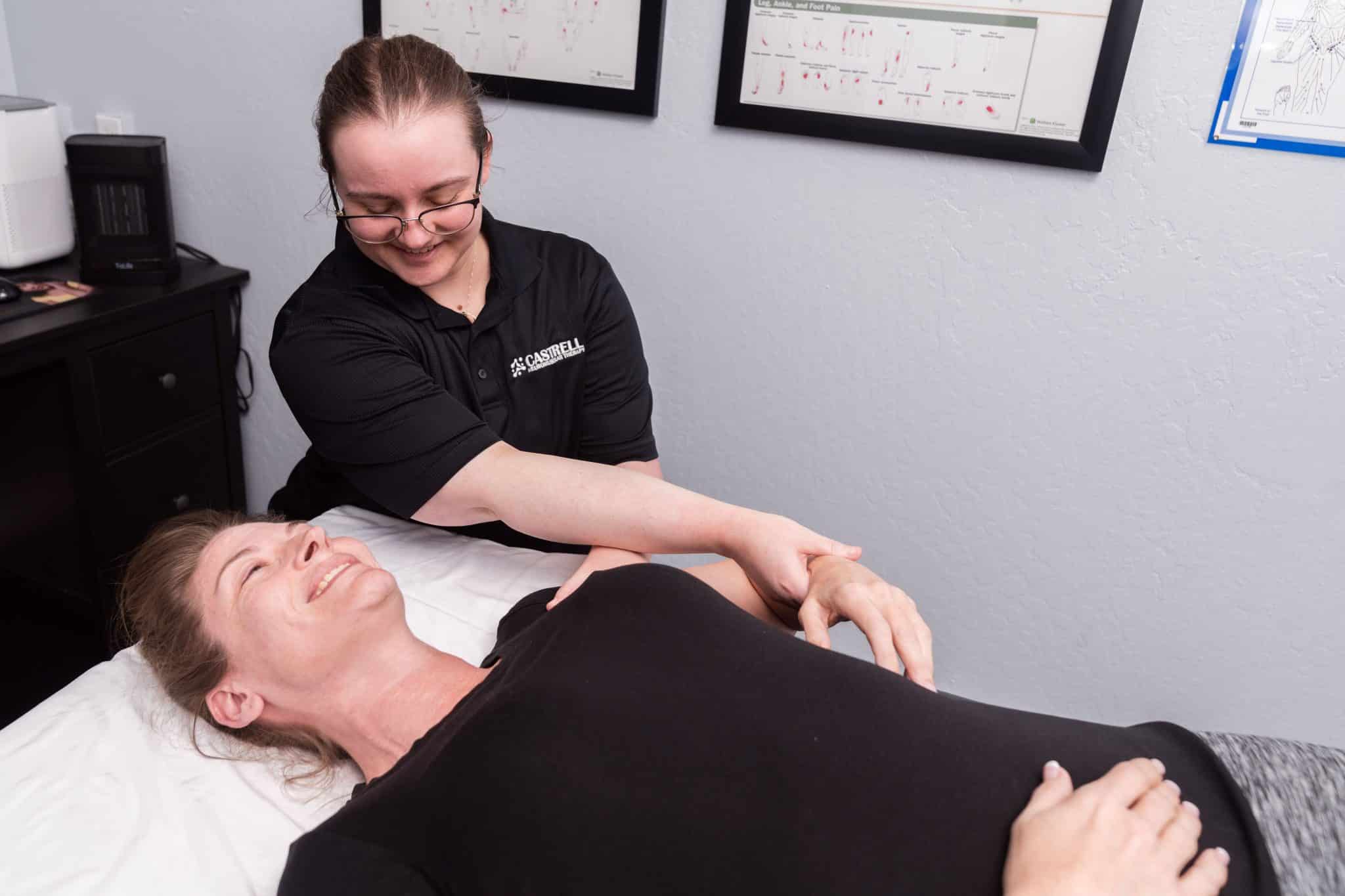
Shoulder Pain
By focusing on the whole person, not just the shoulder, we can provide more effective and lasting relief from shoulder pain, helping our patients return to their everyday activities pain-free.
What Is Shoulder Pain?
Shoulder pain is a common issue that affects many individuals, often arising from various causes such as poor posture, repetitive strain, or even traumatic injury. The shoulder is a highly mobile joint that allows for a wide range of motion, but this flexibility can also make it vulnerable to stress and strain. Dysfunction in the hands, for example, can lead to compensatory overuse of the shoulders, causing discomfort and pain. Similarly, incorrect breathing patterns can affect how the scapula moves around the rib cage, potentially causing improper shoulder movement.
Shoulder pain can also result from a lack of muscular development in the hands or forearms. For example, if someone has well-developed shoulders but underdeveloped hands, they may rely more heavily on their shoulders for tasks, leading to overuse. Shoulder pain can be complex, as its root cause may not always be limited to the shoulder itself. Whether due to injury, muscle dysfunction, or other factors, addressing shoulder pain requires a comprehensive approach to identify the underlying causes and provide effective treatment.
What Are The Symptoms Of Shoulder Pain?
Shoulder pain can manifest in a variety of ways, depending on its cause and severity. Common symptoms include pain in the shoulder joint, which may radiate into the upper arm or neck. This pain can be dull and achy or sharp and sudden, especially when moving the arm above the head or lifting heavy objects.
Another common symptom is stiffness, which limits the range of motion and can make simple tasks like reaching for an item on a high shelf or getting dressed challenging. In more severe cases, individuals may experience weakness in the shoulder or arm, making it difficult to perform everyday activities. Pain during certain movements, such as reaching behind the back or lifting the arms, can also be a clear indication of shoulder dysfunction.
If left untreated, shoulder pain can significantly affect daily life, including activities like lifting children, playing sports, or even performing basic tasks like pouring a cup of coffee. Addressing shoulder pain early is key to preventing further limitations and ensuring long-term recovery.
What Is Our Approach To Fixing/Treating Shoulder Pain?
At Castrell Neuromuscular Therapy, treating shoulder pain starts with a thorough evaluation to identify the root cause of the issue. We believe in looking at the whole body, as shoulder pain often stems from problems not just in the shoulder itself, but also in other areas of the body. This includes evaluating hand function, posture, breathing patterns, and even lower body mechanics. By taking a comprehensive approach, we ensure that we address all potential factors contributing to the pain.
For example, we often see patients who have shoulder pain due to overuse or muscle imbalances in the hands or upper body. In these cases, we help patients focus on strengthening and improving the function of the hands and arms to relieve strain on the shoulders. Additionally, breathing patterns play a significant role in shoulder movement, and poor breathing can affect scapular mobility, leading to improper shoulder movement.
Once we’ve identified the root cause, our treatment includes a range of techniques such as deep tissue massage, joint mobilizations, and thermal therapy, depending on the severity of the pain. For more advanced cases, we may incorporate shockwave therapy to promote healing and oxygenation to the affected tendons, helping to speed up recovery.
We also regularly re-evaluate our patients to track their progress, adjusting the treatment plan as necessary to ensure optimal outcomes. By focusing on the whole person, not just the shoulder, we can provide more effective and lasting relief from shoulder pain, helping our patients return to their everyday activities pain-free.
Download Free Report
Is shoulder pain restricting your ability to do everyday activities and limiting the quality of your life? This free, comprehensive guide is designed to provide you with actionable tips and strategies to reduce discomfort and improve your quality of life. Learn about common causes of shoulder pain, effective treatments, and simple exercises you can start today to feel better. Don’t let pain hold you back any longer – take the first step towards a pain-free life. Download your FREE report now and discover how to regain control and move without limitations!